This article was originally published in Domus 1050, November 2020.
Within months the Covid-19 pandemic has impressed a dramatic impact on societies and economies around the world.
Responses to the crisis have revealed sharp differences in terms of the economic resilience of countries, the social contracts between people and their governments, and the readiness of their institutions, especially health systems. Some countries have found themselves better prepared to coordinate their response and leverage a wide range of capabilities across their ecosystem of hospitals, universities, testing labs and manufacturing enterprises.
During the first wave of the global outbreak, ventilators and essential protective equipment were in shortage in countries like the United Kingdom and Italy, and the fast-growing global demand made it clear that unprecedented action was necessary. Governments set up several mission-oriented challenges around which public and private actors across the national spectrum were asked to identify and coordinate their efforts. While important successes have been achieved, the design and manufacturing journeys presented significant and unexpected challenges.
At the onset of the pandemic, the UK’s National Health Service (NHS) had only 8,000 ventilators, with epidemiological models suggesting the need for 30,000 in a matter of weeks. The UK Government launched the Ventilator Challenge UK consortium on 14 March. The consortium included leading industrial, technology and engineering businesses spanning the aerospace, automotive and medical sectors. Companies in these areas rely on similar technology platforms, flexible supply chains made of highly specialised suppliers, and coherent design capabilities for all product systems. These firms work with ecosystems as much as products.
The High Value Manufacturing Catapult took a coordinating role, especially in the investigation of a range of design options and specifications for a Rapidly Manufactured Ventilator System developed by clinicians and the Medicines and Healthcare Products Regulatory Agency.
This investigation process would normally take months, if not years, given the complex interdependencies between design solutions, technological readiness and manufacturing issues, along the entire innovation and production chains. In times of crisis, the rapid scaling up of design solutions presents even greater challenges. Fighting against time, between parallel and competing projects, different companies (often specialised in non-medical fields) partnered to develop a prototype within weeks.
In times of crisis, the rapid scaling up of design solutions presents even greater challenges
While many firms attempted to develop completely new designs, one group built on product architectures and proven solutions. Many of those who pursued a start-from-scratch approach underestimated the fact that the device’s safety is not merely a design property. Rather, it depends on how the equipment is manufactured, its quality management, and the appropriateness of the product design’s innovation in meeting clinical needs. Shepherding this process by enabling smart shortcuts and shared insights, without generalised assumptions clouding invention, is a delicate balancing act.
The traditional approach of calls and competitions does not generally lead to the intense collaboration required in such situations (it typically generates competition instead), nor does the existing positioning of the innovation funding agency tend to be close enough to the rapidly moving front lines in order to learn and guide.
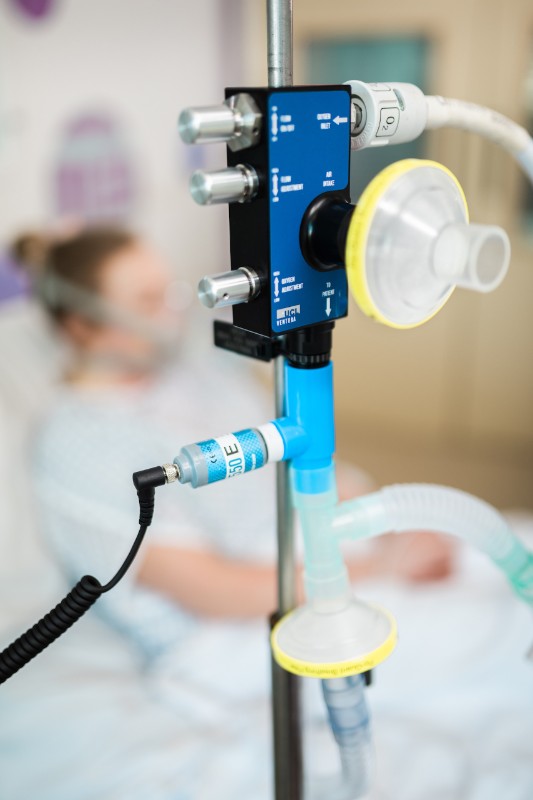
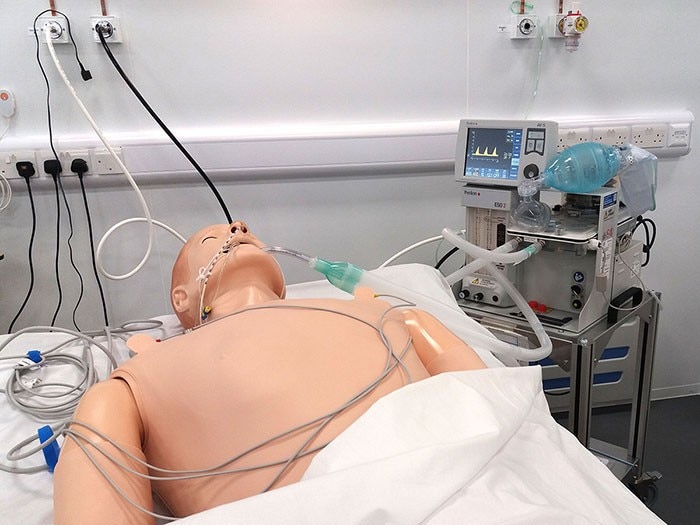
Equally, a novel virus means a constantly changing context. In April, new clinical needs emerged that rendered a number of initial design solutions unsuitable. Covid-19 patients commonly suffer from rapid fluid build-up in the lungs, thus ventilators must allow for frequent drainage. In some cases a number of medical ventilators had to be sent back to manufacturing facilities for retrofitting, leading to delays. The production ramp-up centred ultimately on two design solutions: the Penlon Prima ESO 2 device and the paraPAC plus. The consortium managed to increase the combined capacity of Penlon and Smiths from 50 or 60 ventilators per week, to 100 or 200 per day. By 5 July the consortium concluded after delivering 13,347 ventilators to the NHS.
In Italy, in late March, an alternative design response to the shortage of ventilators arrived from the bottom up.
Doctors at the Sant’Orsola Hospital in Bologna seized the opportunity to effectively double the existing stock of ventilators by designing a circuit through which one device could be used to ventilate two people simultaneously. This would have remained simply an idea if the industrial ecosystem in the Emilia-Romagna region had not been able to produce a functioning “double ventilator” prototype in just three days. The biomedical district in Mirandola has developed design capabilities in medical equipment ranging from disposables to complex haemodialysis machines. These devices feature critical apparatus including flow and fluidic systems, sensors and embedded software, valves and filtration components. Given their complex architecture, integration capabilities and product design modularisation are imperative.
A multidisciplinary approach, building on the engineering but adding richer forms of design capability, may have unlocked a richer set of solutions
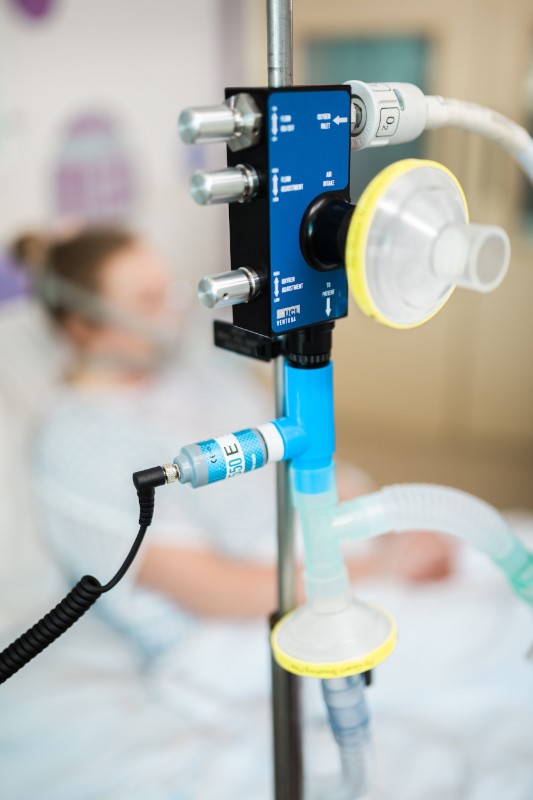
The shortage of ventilators also led to innovative design solutions along different therapeutic lines, namely the increasing use of continuous positive airway pressure (CPAP) devices. Unlike ventilators, CPAP machines deliver oxygen via a mask and do not require intubation. A team at University College London (UCL) launched the UCL-Ventura Initiative for breathing aids in March. Working with industry partners Mercedes AMG High Performance Powertrains, and relying on direct access to clinicians at the UCL Hospital, the Ventura Initiative spawned the production of 10,000 devices in 1 month and over 1,900 open licences across 105 countries.
The original design from 1992 entailed a purely mechanical device simply controlled by rotary valves to alter oxygen concentration and flow rate. While the product was far more straightforward than a ventilator, the UCL team would not have been able to scale up the CPAP without an industrial partner.
The reverse engineering process relied on computer-aided design and computational fluid mechanics simulators, normally used for Formula 1 engine design. Design improvements were constrained by the availability of consumables, later manufactured by Intersurgical.
The product design effort also faced an implementation challenge, determined by the limited supply of oxygen in British hospitals. The Ventura team modelled oxygen flows to each floor and bed area of the UCL Hospital, hence designing an integrated product-system-therapy solution.

For protective equipment with simple product design such as disposable masks, design capabilities were mainly required in developing robust and highly automated manufacturing technologies and processes capable of delivering high-volume production over sustained periods. In Italy the shortage of masks, for example, was addressed by a leading packaging machinery company called IMA S.p.A. Responding to a call from the Italian government, the company was able to design a streamlined and highly flexible production line – IMA Face 400 – able to produce (and package) between 200 and 400 masks per minute.
The design of 25 machines capable of satisfying national demand was piloted by an agile task force leveraging both internal design and organisational capabilities, as well as a network of specialised contractors providing components despite lockdown restrictions. A resilient supply chain was critical in finding the most appropriate process and product system design solutions.
Le soluzioni di progettazione emerse durante la pandemia ci hanno fornito numerose lezioni
The context of such technologies is accessed via different design disciplines, such as the trio of interaction design, service design and strategic design. Taking a multidisciplinary approach – building on the engineering but adding richer forms of design capability – may have unlocked a richer set of other solutions. Such responses could be more immediately effective, cheaper, faster to deploy, easier to use for both medical staff and patients, and with a sensitivity to cultural diversity necessary in such contexts.
Engineering-led approaches do not tend to deal with these aspects. Equally, strategic design would ensure that broader insights would be generated, such as how the efficiency-oriented “just-in-time” supply chain and procurement logics came to dominate healthcare in the first place, particularly in the UK.
These wider questions can be addressed by design, and are crucial to building true resilience, or at least learning from a crisis. But they are unlikely to emerge from a Ventilator Challenge launched by a High Value Manufacturing Catapult. As is often the case, an all-too-simplistic focus on science, technology and engineering develops blind spots around the more ambiguous, yet equally productive, aspects of culture, policy and politics. While ventilators needed to be produced quickly, the broader issue of why ventilators were not there to begin with also needs addressing. That is not an engineering problem, but it can be addressed by different forms of design.

Several lessons have been learnt from various design and manufacturing initiatives that emerged during the pandemic. The Covid-19 emergency has ultimately revealed how the development and diffusion of design capabilities in the health sector is at the core of both the innovation ecosystem and the choices we have made about the everyday infrastructures comprising healthcare. In both cases, forms of design can help improve the resilience of societies and economies in times of crisis.
Part of this design challenge concerns solutions that are functionally appropriate and affordable. A further challenge would be to address the broader policy contexts that produce – or diminish – such resilient solutions. Developing this richer set of design capabilities, well beyond engineering, can generate health technologies tuned to people and place, allowing us to address both the short and long-term emergencies we now face.
Antonio Andreoni works at the Institute for Innovation and Public Purpose, University College London.
Dan Hill works at the Institute for Innovation and Public Purpose, University College London, and Vinnova, Sweden.